by Dr. Manaan Kar Ray
NOTICE: THIS WORK MAY BE PROTECTED BY COPYRIGHT
YOU ARE REQUIRED TO READ THE COPYRIGHT NOTICE AT THIS LINK BEFORE YOU READ THE FOLLOWING WORK, THAT IS AVAILABLE SOLELY FOR PRIVATE STUDY, SCHOLARSHIP OR RESEARCH PURSUANT TO 17 U.S.C. SECTION 107 AND 108. IN THE EVENT THAT THE LIBRARY DETERMINES THAT UNLAWFUL COPYING OF THIS WORK HAS OCCURRED, THE LIBRARY HAS THE RIGHT TO BLOCK THE I.P. ADDRESS AT WHICH THE UNLAWFUL COPYING APPEARED TO HAVE OCCURRED. THANK YOU FOR RESPECTING THE RIGHTS OF COPYRIGHT OWNERS.
A combination of psychological and biological etiological processes along with the person's psychological history, the nature of the trauma, and the availability of posttrauma support go on to decide the absence or presence of PTSD symptoms in a person after a traumatic event. The risk factors have been enumerated beneath, however it must be borne in mind that someone without risk factors who is exposed to a traumatic event ,may also develop symptoms.
Demographic Risk Factors:
• Women being at a greater risk than men
• Black and Hispanic being at a greater risk than Caucasian
Pretrauma Risk Factors include:
• previous trauma (childhood sexual or physical abuse)
• childhood separation from parents
• family instability
• a predisposing mental health condition (anxiety or depression)
• the type and severity of the traumatic event
• lack of adequate and competent support for the person after the trauma.
The psychological history of a person may include risk factors for developing PTSD after a traumatic event:
• Borderline personality and/or dependent personality disorders
• Low self-esteem
• Neuroticism
• Pre-existing negative beliefs
• Previous trauma
People with borderline personality disorder often have a history of physical and/or sexual abuse, neglect, hostile conflict, and parental loss or separation. Dependent personality disorder is characterized by low self-esteem, fear of separation, and the excessive need to be cared for by others. All of these features may predispose someone for PTSD after experiencing a traumatic event.
People who have experienced previous trauma(s) are at risk for developing PTSD. Repeated exposure to trauma causes hyperactive release of stress hormones, which may be instrumental in creating symptoms of PTSD.
Trauma-Related Risk Factors
The severity, duration, proximity to (direct or witnessed), and type of traumatic event are the most significant risk factors for developing PTSD. Directly experienced traumatic events include the following examples:
• Combat
• Kidnapping
• Natural disasters (e.g., fire, tornado, earthquake)
• Catastrophic accident (e.g., auto, airplane, mining)
• Violent sexual assault
• Violent physical assault
Witnessed traumatic events include the following examples:
• Seeing another person violently killed or injured
• Unexpectedly seeing a dead body or body parts
Whether or not the event was perpetrated in a sadistic manner (e.g., torture, rape) occurred accidentally (e.g., fire), or occurred as an "act of God" can affect whether a person develops PTSD and whether the disorder is acute, chronic, or has a delayed onset of symptoms.
Posttrauma Risk Factors
Symptoms and duration of PTSD may be more severe if there is a lack of support from family and/or community. For instance, a rape victim who either is blamed for the assault or not believed (e.g., in the case of rape by a family member) may be at greater risk for developing PTSD.
Symptoms & Complications:
Symptoms of PTSD are generally of three types:
• Intrusive (Re-experiencing the trauma)
o Recurrent recollections associated with distress
o Intrusive emotions and memories
o Dissociative states
o Flashbacks
o Nightmares and night terrors
• Avoidant
o Avoiding emotions
o Avoiding relationships
o Avoiding responsibility for others
o Avoiding situations that are reminiscent of the traumatic event
o Inability to recall an important aspect of the trauma
o Diminished interest or participation in activities
o Restricted range of affect
o Sense of foreshortened future
• Hyperarousal
o Exaggerated startle reaction
o Explosive outbursts
o Extreme vigilance
o Irritability
o Difficulty concentrating
o Panic symptoms
o Sleep disturbance
Re-experiencing symptoms:
One set of PTSD symptoms involves persistent and distressing re-experiencing of the traumatic event in one or more ways. In these symptoms, the trauma comes back to the PTSD sufferer in some way, through memories, dreams, or distress in response to reminders of the trauma. A more extreme example of this is "flashbacks," where individuals feel as if they are reliving the traumatic experience. For example, the sounds and images of combat often comprise the content of flashbacks experienced by military veterans. Flashbacks can be triggered by ordinary stimuli such as a low-flying airplane or a loud noise, anything that brings to mind an aspect of the event. PTSD is distinguished from "normal" remembering of past events by the fact that re-experiencing memories of the trauma(s) are unwanted, occur involuntarily, elicit distressing emotions, and disrupt the functioning and quality of life of the individual. PTSD may even give rise to dissociative symptoms including psychic numbing, depersonalization, and amnesia.
Avoidance and numbing symptoms:
A second set of PTSD symptoms involves persistent avoidance of stimuli associated with the trauma, and numbing of general responsiveness. These symptoms involve avoiding reminders of the trauma. Reminders can be internal cues, such as thoughts or feelings about the trauma, and/or external stimuli in the environment that spark unpleasant memories and feelings. To this limited extent, PTSD is not unlike a phobia, where the individual goes to considerable length to avoid stimuli that provoke emotional distress. PTSD symptoms also involve more general symptoms of impairment, such as pervasive emotional numbness, feeling "out of sync" with others, or a lack of expectation for future goals being met, due to their trauma experiences.
Symptoms of increased arousal:
This set of symptoms is represented by persistent symptoms of increased arousal not present before the trauma. These symptoms can be apparent in difficulty falling or staying asleep, irritability or outbursts of anger, difficulty concentrating, a hypervigililant watchfulness, and/or an exaggerated startle response. Individuals suffering from PTSD experience heightened physiological activation, which may occur in a general way, even while at rest. More typically, this activation is evident as excessive reaction to specific stressors that are directly or symbolically reminiscent of the trauma. This set of symptoms is often, but not always, linked to reliving of the traumatic event. For example, sleep disturbance may be caused by nightmares, intrusive memories may interfere with concentration, and excessive watchfulness may reflect concerns about preventing recurrence of a traumatic event that may be similar to that previously endured.
Complications:
Complications develop in people with chronic PTSD and delayed onset PTSD. These include the following:
• Alcohol and drug abuse or dependence
• Chronic anxiety
• Depression and increased risk for suicide
• Divorce and separation
• Guilt
• Low self-esteem
• Panic attacks
• Phobias
• Unemployment
In 1988, it was estimated that 40% of Vietnam veterans had problems with drug abuse, and almost one-half of these veterans had been divorced at least once.
Phobias of objects, situations, or environments that remind the person of the event often develop as complications of PTSD.
Panic attacks can be triggered by stimuli reminiscent of the event.
People with chronic PTSD and complications often become unemployed because severe symptoms interfere with their ability to perform their jobs and function socially in the workplace.
Diagnosis
There is no laboratory test for PTSD. The diagnosis is based on the clinical history of the patient and the occurrence of a traumatic event. A diagnosis of PTSD cannot be made without a clear history of a traumatic event.
The American Psychiatric Association (APA) specifies the symptoms and criteria for PSTD in its Diagnostic and Statistic Manual of Mental Disorders:
Diagnostic Criteria for Post-Traumatic Stress Disorder:
A. The person has been exposed to a traumatic event in which both of the following were present:
1. The person experienced, witnessed, or was confronted with an event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others.
2. The person’s response involved intense fear, helplessness, or horror. Note: In children, this may be expressed instead by disorganized or agitated behavior.
B. The traumatic event is persistently re-experienced in one (or more) of the following ways:
1. Recurrent and intrusive distressing recollections of the event, including images, thoughts, or perceptions. Note: In young children, repetitive play may occur in which themes or aspects of the trauma are expressed.
2. Recurrent distressing dreams of the event. Note: In children, there may be frightening dreams without recognizable content.
3. Acting or feeling as if the traumatic event were recurring (includes a sense of reliving the experience, illusions, hallucinations, and dissociative flashback episodes, including those that occur on awakening or when intoxicated). Note: In young children, trauma-specific reenactment may occur.
4. Intense psychological distress at exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
5. Physiological reactivity on exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
C. Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness (not present before the trauma), as indicated by three (or more) of the following:
1. Efforts to avoid thoughts, feelings, or conversations associated with the trauma.
2. Efforts to avoid activities, places, or people that arouse recollections of the trauma
3. Inability to recall an important aspect of the trauma
4. Markedly diminished interest or participation in significant activities
5. Feeling of detachment or estrangement from others
6. Restricted range of affect (e.g., unable to have loving feelings)
7. Sense of a foreshortened future (e.g., does not expect to have a career, marriage, children, or a normal life span)
D. Persistent symptoms of increased arousal (not present before the trauma), as indicated by two (or more) of the following:
1. Difficulty falling or staying asleep
2. Irritability or outbursts of anger
3. Difficulty concentrating
4. Hypervigilance
5. Exaggerated startle response
E. Duration of the disturbance (symptoms in Criteria B, C, and D) is more than 1 month.
F. The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
APA. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. 1994. Washington, DC: American Psychiatric Association (APA).
Several semistructured interviews assess the DSM IV criteria for PTSD like Structured Clinical Interview for DSM IV (SCID), And the Anxiety Disorders Interview Schedule for DSM IV (AIDS-IV). Another tool used to evaluate symptoms of PTSD is the Clinician-Administered PTSD Scale (CAPS), a self-reporting questionnaire that assesses the nature of trauma, the patient's current condition, and the prognosis. The CAPS also helps identify associated conditions or complications, such as guilt and an impaired sense of surroundings.
Differential Diagnosis:
Other conditions cause many of the symptoms experienced in PTSD and these conditions must be ruled out. Additionally, conditions such as substance abuse and depression develop as complications of PTSD. Ultimately, the distinguishing factor is the fact that the patient has experienced a severe trauma.
Some of the conditions that must be ruled out include the following:
• Acute stress disorder (duration of upto 4 weeks)
• Adjustment disorder (less severe stressor or different symptom pattern)
• Mood disorder or other anxiety disorder (symptoms of avoidance, numbing, or hyperarousal present before exposure to the stresor)
• Other disorders with intrusive thoughts or perceptual disturbances (e.g. obsessive compulsive disorder, schizophrenia, other psychotic disorder)
• Substance abuse or dependence disorder
Furthermore, malingerers — that is, people who falsely claim to be traumatized—sometimes feign PTSD symptoms in order to win money in a court case as compensation for "emotional suffering."
Course:
The course of PTSD is often determined on when the person begins to experience symptoms.
Immediate Onset:
• Better response to treatment
• Better prognosis (i.e., less severe symptoms)
• Fewer associated symptoms or complications
• Symptoms are resolved within 6 months
Delayed Onset:
• Associated symptoms and conditions develop
• Condition more likely to become chronic
• Possible repressed memories
• Worse prognosis
People who experience trauma sometimes repress their memories of the event to avoid the pain of thinking about or remembering them. These so-called repressed memories sometimes resurface during therapy or may be triggered by something in everyday experience that reminds the patient of the traumatic event.
Working with repressed memories in therapy is controversial, because many therapists doubt their validity and accuracy. Repressed memories are typically retrieved during hypnosis, which many psychiatrists consider an unreliable tool for memory exploration.
About 50% of those who have acute onset of symptoms recover within 6 months. Roughly 30% develop chronic symptoms that may affect them for the rest of their lives. Others experience intermittent periods of symptom severity and remission.
Treatment -- Psychotherapy:
A combination of psychotherapy and medication is commonly used to treat PTSD. Brief descriptions of the various treatment modalities have been provided herewith for a better understanding of intervention in suffering patients.
Treatment for PTSD typically begins with a detailed evaluation, and development of a treatment plan that meets the unique needs of the survivor. Generally, PTSD-specific-treatment is begun only when the survivor is safely removed from a crisis situation. For instance, if currently exposed to trauma (such as by ongoing domestic or community violence, abuse, or homelessness), severely depressed or suicidal, experiencing extreme panic or disorganized thinking, or in need of drug or alcohol detoxification, addressing these crisis problems becomes part of the first treatment phase.
The following intervention principles are common in most cases:
• Educating trauma survivors and their families about how persons get PTSD, how PTSD affects survivors and their loved ones, and other problems that commonly come along with PTSD symptoms. Understanding that PTSD is a medically recognized anxiety disorder that occurs in normal individuals under extremely stressful conditions is essential for effective treatment.
• Examining and resolving strong feelings such as anger, shame, or guilt, which are common among survivors of trauma
• Teaching the survivor to cope with post-traumatic memories, reminders, reactions, and feelings without becoming overwhelmed or emotionally numb. Trauma memories usually do not go away entirely as a result of therapy, but become manageable with new coping skills.
Psychotherapy:
Psychotherapeutic treatments include the following:
• Debriefing (i.e., crisis intervention)
• Cognitive Behavioral Therapy
• Group Psychotherapy
• Brief Psychodynamic Psychotherapy
• Eye movement desensitization and reprocessing (EMDR)
• Hypnotherapy
Debriefing sessions are usually conducted as soon after the event as possible. The session usually lasts about 2 hours. A debriefing session typically involves a discussion of the event, the person's reaction to it, and coping strategies. Debriefing sessions are commonly used to help rescue personnel, classmates of students who die in auto accidents or as a result of a violent attack (e.g., victims of random shootings), and survivors of terrorist attacks (e.g., bombings of public buildings).
Psychotherapy is generally necessary in the treatment of PTSD, whether it is conducted in individual therapy or in "survivor group" therapy. Survivor groups may be associated with or may refer group members to local community agencies that offer therapy and support for victims of rape, domestic violence, combat, natural disasters, and so on.
The goal of psychotherapy in the treatment of PTSD is to help the person address and manage painful memories until they no longer cause disabling symptoms. This begins after establishing a safe relationship between the client and therapist. The process involves gradually working through the traumatic event and the patient's reactions to it, validating the patient's experiences, repairing damage done to their identity, and dealing with loss.
Cognitive-behavioral therapy (CBT) involves working with cognitions to change emotions, thoughts, and behaviors. Exposure therapy, is one form of CBT unique to trauma treatment which uses careful, repeated, detailed imagining of the trauma (exposure) in a safe, controlled context, to help the survivor face and gain control of the fear and distress that was overwhelming in the trauma. In some cases, trauma memories or reminders can be confronted all at once ("flooding"). For other individuals or traumas it is preferable to work gradually up to the most severe trauma by using relaxation techniques and either starting with less upsetting life stresses or by taking the trauma one piece at a time ("desensitization").
Along with exposure, CBT for trauma includes learning skills for coping with anxiety (such as breathing retraining or biofeedback) and negative thoughts ("cognitive restructuring"), managing anger, preparing for stress reactions ("stress inoculation"), handling future trauma symptoms, as well as addressing urges to use alcohol or drugs when they occur ("relapse prevention"), and communicating and relating effectively with people ("social skills" or marital therapy).
Group treatment is often an ideal therapeutic setting because trauma survivors are able to risk sharing traumatic material with the safety, cohesion, and empathy provided by other survivors. As group members achieve greater understanding and resolution of their trauma, they often feel more confident and able to trust. As they discuss and share coping of trauma-related shame, guilt, rage, fear, doubt, and self-condemnation, they prepare themselves to focus on the present rather than the past. Telling one's story (the "trauma narrative") and directly facing the grief, anxiety, and guilt related to trauma enables many survivors to cope with their symptoms, memories, and other aspects of their lives.
Brief psychodynamic psychotherapy focuses on the emotional conflicts caused by the traumatic event, particularly as they relate to early life experiences. Through the retelling of the traumatic event to a calm, empathic, compassionate and non-judgmental therapist, the survivor achieves a greater sense of self-esteem, develops effective ways of thinking and coping, and more successfully deals with the intense emotions that emerge during therapy. The therapist helps the survivor identify current life situations that set off traumatic memories and worsen PTSD symptoms.
Eye movement desensitization and reprocessing (EMDR) is a specialized form of psychotherapy that is used almost exclusively for treating PTSD and its associated conditions, including depression. EMDR typically is integrated into a conventional psychotherapy regimen and is not used alone to treat PTSD. It involves elements of exposure therapy and cognitive behavioral therapy, combined with techniques (eye movements, hand taps, sounds) which create an alteration of attention back and forth across the person's midline.
The theory behind EMDR is that stimulated rapid eye movement may help in the psychological processing of trauma. It is thought that the day’s events and our reactions to them are processed during REM sleep . In a controlled EMDR session, moving light is used to induce rapid eye movement.
Because it is a new method of treatment, only a relatively small number of patients have been treated with EMDR for PTSD. However, the EMDR Institute reports that there are more controlled studies of EMDR and its effects than of any other trauma treatment. The EMDR Institute states that an estimated 1,000,000 people had been treated by 1995, with varying degrees of improvement. Some, but not all, studies document improvement after relatively few interventions.
Hypnotherapy involves giving instructions to the patients to induce a state of highly focused attention, a reduced awareness of peripheral stimuli, and a heightened suggestibility. The goal of this treatment is to enhance control over trauma-related emotional distress and hyperarousal symptoms and to facilitate the recollection of details of the traumatic event.
Treatment -- Pharmacotherapy:
Pharmacotherapy:
The use of medication in addition to psychotherapy has been shown to be beneficial in the treatment of PTSD. Treatment is symptom related and essnetially depends on one of the following groups of drugs:
• Selective Serotonin Reuptake Inhibitors
• Serotonin and Noradrenaline Reuptake Inhibitors
• Tricyclic antidepressant
• Anxiolytics
Selective Serotonin Reuptake Inhibitors (SSRIs)
Based on the research evidence, SSRI antidepressants are the best first-line treatment for PTSD. The five SSRIs available in the United States are:
Right now one medication, sertraline (Zoloft), has FDA approval for treating PTSD. In Great Britain however Paroxetine (Seroxat) is the only one that is approved for use in PTSD. Other medications in the SSRI class are also probably effective—in fact, if one SSRI is ineffective or has intolerable side effects, a second SSRI may prove beneficial and well tolerated.
Serotonin is a neurotransmitter that helps transfer information from one brain cell (neuron) to another. Imbalances in serotonin are thought to play a major role in causing or continuing PTSD. Antidepressant medications may work by correcting these imbalances. The antidepressants known as SSRIs are unlike most other antidepressants in that they have little effect on neurotransmitters other than serotonin. Although quite different in their chemical structures, these medications share the property of inhibiting serotonin reuptake, so their modes of action and side effects are similar.
Serotonin and Noradrenaline Reuptake Inhibitors (SNRIs)
High-dose nefazodone (Serzone®) therapy may help control intrusive and hyperarousal symptoms. In fact both nefazodone (Serzone) and venlafaxine (Effexor) have shown promise as second-line treatment if SSRIs prove ineffective or are not well tolerated. They have a more favorable side-effect profile than the tricyclics.
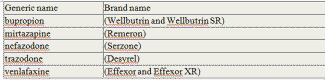
While nefazodone (Serzone) and venlafaxine (Effexor and Effexor XR) are the recommended second-line medications for PTSD, it is possible that other antidepressants may also be helpful. We include them here because clinicians may prescribe them. These medications include:
Tricyclic antidepressants (TCA):
TCAs (e.g., clomipramine [Anafranil®]; doxepin [Sinequan®]) could be employed if the person has had a good response to them in the past and they do not cause too many side effects, or if the person has failed to respond to or does not tolerate the SSRIs, nefazodone or venlafaxine. They have been shown to reduce insomnia and dream disturbance, anxiety, guilt, flashbacks, and depression. Mood stabilizers (Lithium) may be added to improve a partial response to an antidepressant.
Anxiolytics (antianxiety agents):
Anxiolytics including benzodiazepines (e.g., diazepam [Valium®]; chlordiazepoxide [Librium®]) are ideally used only briefly and intermittently, if at all, to quell acute and severe anxiety symptoms. While they reduce anxiety rapidly, they also often induce sedation, impaired coordination and the development of physical dependency in those who use them for more than a few weeks and usually are not recommended as treatment for PTSD, because patients with this disorder are often predisposed to developing substance abuse. Gabapentin (Neurontin) is sometimes used in the place of benzodiazepines because it has similar benefits and does not cause dependency. Unfortunately, it is quite expensive. Buspirone [BuSpar®] has been shown to reduce anxiety, irritability, insomnia, and hypervigilance. However no studies have been done demonstrate long-term effectiveness.
Anticonvulsants:
Anticonvulsants (Carbamazepine and Valproate) have shown promising effects in preliminary studies.
