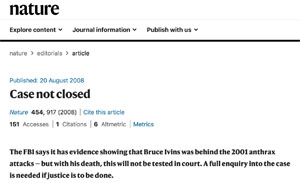
Viet Thanh Nguyen on Roots of Anti-Asian Hate from U.S. Colonialism to Anti-China Political Rhetoricby Amy Goodman
Democracy Now
MARCH 22, 2021Watch Full Show
https://www.democracynow.org/2021/3/22/ ... a_killingsGUESTS
Viet Thanh Nguyen: Pulitzer Prize-winning author and professor at the University of Southern California.
LINKS
Viet Thanh Nguyen on Twitter
"Bipartisan political rhetoric about Asia leads to anti-Asian violence here""The Committed"Protests condemning hate crimes against Asian Americans continue, following the deadly shootings in Atlanta where a white gunman attacked three Asian-owned spas and killed eight people, six of them women of Asian descent. Hundreds of people gathered outside the Georgia state Capitol in Atlanta and around the U.S. demanding an end to anti-Asian racism and honoring the lives of the eight people who were killed: Xiaojie Tan, Yong Ae Yue, Delaina Ashley Yaun, Suncha Kim, Hyun Jung Grant, Soon Chung Park, Daoyou Feng and Paul Andre Michels. Anti-Asian hate in the United States is “not anything new,” says Viet Thanh Nguyen, a Pulitzer Prize-winning Vietnamese American writer. “The history of anti-Asian violence in this country goes back to as long as we’ve had Asian immigrants in this country.” He also speaks about the dangers of anti-China rhetoric from both Republican and Democratic leaders and how that contributes to suspicion of Asian Americans.
Transcript
This is a rush transcript. Copy may not be in its final form.
AMY GOODMAN: This is Democracy Now!, democracynow.org, The Quarantine Report. I’m Amy Goodman.
Protests condemning racism and hate crimes against Asian Americans continue, following last week’s deadly shootings in Atlanta, where a white 21-year-old gunman attacked three Asian-owned spas, killing eight people, seven of them women, six of them women of Asian descent.
President Biden and Kamala Harris traveled to Atlanta on Friday to meet with Asian American leaders. Vice President Harris, who is the the first Asian American and first woman vice president, condemned last week’s attacks.
VICE PRESIDENT KAMALA HARRIS: Whatever the killer’s motive, these facts are clear: Six out of the eight people killed on Tuesday night were of Asian descent. Seven were women. The shootings took place in businesses owned by Asian Americans. The shootings took place as violent hate crimes and discrimination against Asian Americans has risen dramatically over the last year and more. In fact, over the past year, 3,800 such incidents have been reported, two of three by women, everything from physical assaults to verbal accusations. And it’s all harmful. And sadly, it’s not new. Racism is real in America, and it has always been. Xenophobia is real in America and always has been. Sexism, too. … For the last year, we’ve had people in positions of incredible power scapegoating Asian Americans, people with the biggest pulpits spreading this kind of hate.
AMY GOODMAN: On Saturday, hundreds of demonstrators gathered outside the Georgia state Capitol in Atlanta. Speakers included Georgia state Representative Bee Nguyen.
REP. BEE NGUYEN: We have lived in the shadows, invisible, overlooked, stereotyped and relegated as second-class citizens. And now, in the wake of a violent and brutal shooting, white America is still trying to deny our humanity and existence. A 21-year-old white man targeted three Asian businesses, driving 40 minutes from one spot to another, passing other adult entertainment businesses, but he shot and killed eight people, six of them being Asian women, at close range, in the head. No matter how you want to spin it, the facts remain the same. This was an attack on the Asian community.
AMY GOODMAN: The Reverend William Barber, co-founder of the Poor People’s Campaign, also addressed the protest in Atlanta.
REV. WILLIAM BARBER II: Let us not forget that white supremacy is not just against Black people, but humanity itself. Let us remember that white supremacy is a form of self-worship and idolatry. And whenever it is pushed and promulgated by presidents and politicians and preachers, it can cause some of the most strangely justification for the taking of life this world has ever seen. And when white supremacy is promulgated, it will try to justify taking Black life, taking Brown life, taking Indigenous life, taking Indian life, taking Asian life, taking Jewish life, taking Muslim life, taking Palestinian life and taking gay life. And we come here to say that white supremacy is a lie teller and a life taker!
AMY GOODMAN: As we continue to look at the mass shootings in Atlanta, the spike in hate crimes targeting Asian Americans and broader issues, we’re joined in Los Angeles, California, by the Pulitzer Prize-winning Vietnamese American writer Viet Thanh Nguyen. His new novel, The Committed, a sequel to his best-selling book, The Sympathizer. His other books include The Refugees and The Displaced: Refugee Writers on Refugee Lives, which he edited. Viet Thanh Nguyen came to the United States as a refugee when he was 4 years old. He’s a professor at the University of Southern California and recently co-wrote an article for The Washington Post headlined “Bipartisan political rhetoric about Asia leads to anti-Asian violence here.”
Professor Nguyen, it’s great to have you back on Democracy Now! Congratulations on your new book! And condolences on the horror that has taken place in Atlanta, which is not just a horror for the Asian American community, but clearly for all of us. If you can talk about the significance of what happened and also the point you make in this op-ed in The Washington Post, where you say, “Bipartisan political rhetoric about Asia leads to anti-Asian violence here”?
VIET THANH NGUYEN: Hi, Amy. Thanks so much for having me back again and to speak on this really tragic topic.
I spent the last week talking to a lot of fellow Asian Americans. We’re all, I think, in a state of anger and despair about what happened, and, I think, partly because, for many of us, we recognize that this is not anything new. As I’ve spoken about repeatedly, and as have so many others, the history of anti-Asian violence in this country goes back to as long as we’ve had Asian immigrants in this country, that Asian immigrants have been brought here to have their labor exploited. And to have that labor exploited, it’s often couched in a language and a justification of racism and sexism.
And that is also tied to the United States’ attitudes towards Asia as a whole, that the United States has, ever since the 19th century, been focused on expanding westwards into Asia, especially China, to reach Asian resources, and that this has had a distinct relationship in terms of pulling Asia immigrants to the United States, either through economic relationships or through wars that the United States has fought with many Asian countries.
So, for many of us, I think, during the last year of the pandemic, to hear President Trump and many of his supporters talk about COVID-19 as the “kung flu” and the “China virus” was simply the most recent manifestation of a deep-held anti-Asian racism, that when people say things like “kung flu” and “China virus,” they’re tapping into this very deep well of anti-Asian feeling. And I think that that combined with the obvious stresses of the pandemic has a direct relationship to the rise, the very significant rise, in anti-Asian violence and rhetoric that many people have experienced in the last 12 months.
But outside of that immediate trigger, I think that the bipartisan rhetoric that I mentioned, the fact that both Democrats and Republicans have focused on China as the major threat and competitor to the United States, number one, continues this concern with Asia that’s been present throughout much of American history, but also keeps China in the foreground of the American imagination as a country to be feared. And I think that, inevitably, whether this is said with explicit racism or just with a latent and implicit xenophobia, it can’t help but to aggravate the suspicions and the feelings of many Americans about people of Asian descent.
AMY GOODMAN: As we speak, in this past week, Secretary of State Antony Blinken and the Pentagon chief, Lloyd Austin, have been traveling the world and fully taking on China, if you will. I mean, Secretary of State Blinken had his first face-to-face meeting with top Chinese officials in Alaska. During a press conference before that with Japanese officials earlier in the week, Blinken warned China not to use coercion or aggression. This is what he said.
SECRETARY OF STATE ANTONY BLINKEN: We’re united in the vision of a free and open Indo-Pacific region, where countries follow the rules, cooperate whenever they can, and resolve their differences peacefully. And in particular, we will push back, if necessary, when China uses coercion or aggression to get its way.
AMY GOODMAN: And this is Defense Secretary Lloyd Austin speaking at that joint news conference in Japan.
DEFENSE SECRETARY LLOYD AUSTIN: I know Japan shares our concerns with China’s destabilizing actions. And as I have said before, China is a pacing challenge for the Department of Defense.
AMY GOODMAN: And so, you have Austin. You have Biden. We’re not just talking about Trump using terms like the “China virus.” Can you respond to what they have been saying?
VIET THANH NGUYEN: Well, I think, again, that much of American foreign policy, during the period of the Cold War and afterwards, has depended upon a foreign other, whether it’s the Soviet Union or China in those years. And it’s obvious, I mean, that we need a foreign other in order to target our political rhetoric, in order to justify our vast expenditures in terms of our military-industrial complex.
So, China has again resumed that position for the United States — Russia, too, to a certain extent. But I think China, because of this, again, deep well of anti-Asian racism, this set of Orientalist expectations that we have that China is going to be mysterious, that it’s going to be menacing, that it’s going to have all kinds of calculations going on strategically and economically that we have to worry about — all this is being put forth by various people in both parties.
And I think that one of the things to stress here is that, of course, there are things about China that we should be concerned about. I think that we should be concerned about human rights abuses that China has undertaken in Tibet, Hong Kong and Xinjiang. But oftentimes this kind of rhetoric about what China is doing is, again, being used to justify an American militaristic stance against China, instead of the United States worrying about how it can compete with China economically but in a nonviolent and nonthreatening manner. And, of course, our outrage about the depredations of China against its own people is sometimes a little bit hypocritical, ,because we’re still struggling, as we are talking about now, with our own capacity to take care of Americans.
AMY GOODMAN: Last week, Republican Congressmember Chip Roy of Texas was rebuked for using a House Judiciary Committee meeting on the rise of anti-Asian violence to glorify lynchings and used rhetoric about China that stokes racism toward Asian American communities. This is just a small part of what he said.
REP. CHIP ROY: I think there’s old sayings in Texas about, you know, find the — all the rope in Texas and get a tall oak tree. … So, now we’re talking about whether talking about China, the Chicoms, the Chinese Communist Party, whatever phrasing we want to use, and if some people are saying, “Hey, we think those guys are the bad guys,” for whatever reason — and let me just say clearly, I do. I think the Chinese Communist Party, running the country of China, I think they’re the bad guys. And I think that they are harming people.
AMY GOODMAN: So, that was Texas Congressmember Chip Roy using the term, the Cold Warrior term, “Chicom,” for the Chinese Communist Party. This was a hearing on violence against Asian Americans. This was the response from New York Democratic Congressmember Grace Meng.
REP. GRACE MENG: Your president and your party and your colleagues can talk about issues with any other country that you want, but you don’t have to do it by putting a bull’s-eye on the back of Asian Americans across this country, on our grandparents, on our kids. This hearing was to address the hurt and pain of our community and to find solutions, and we will not let you take our voice away from us.
AMY GOODMAN: That was Democratic Congressmember Grace Meng. If you, Professor Nguyen, could respond to what he said and what this means?
VIET THANH NGUYEN: Well, again, the reflexive turn from trying to talk about anti-Asian violence within the United States directed against Asian Americans suddenly being undertaken to do a pivot towards this fear of Asia, but also the rhetoric of law and order, of violence, of using lynching, it demonstrates what the Reverend William Barber said in the excerpt of his speech that you talked about, which is that these manifestations of anti-Asian racism are almost inevitably tied towards other manifestations of violence — here, in this case, the specter of lynching brings up anti-Black racism that’s been endemic in this country — and that these domestic manifestations of anti-Asian and anti-Black racism are tied, again, together with justifications for American foreign policy.
Now, the term that the Reverend Barber, William Barber, used was “white supremacy” to connect all of these kinds of manifestations, and I think that that is correct, that for some people in the United States, talking about anti-Asian violence means that it allows them to deploy other methods of violence directed against other kinds of populations, whether it’s populations abroad or, as well, in this case, the idea that African Americans or Black people also need to be suppressed in this country. So I think one of the points that we, as Asian Americans, must insist on is that our efforts are tied together here. You know, our efforts to highlight and to combat anti-Asian racism also need to go hand in hand with the necessity to address anti-Black racism, as well.
AMY GOODMAN: Professor Nguyen, I wanted to ask you about the whole media coverage of what has happened in Atlanta. In that first police news conference last week after the deadly shootings, Cherokee County Sheriff’s Department spokesperson Captain Jay Baker said the 21-year-old shooter Robert Aaron Long’s killing spree was not racially motivated, and instead stemmed from his sex addiction. He said that the young man himself said it wasn’t racially motivated. If you could — now, he’s been removed as the spokesperson now because there was such outcry over what he said. But it has framed the discussion, and the issue of hate crimes has yet to be raised. He certainly hasn’t been charged with them. If you can comment on that and also comment on this issue — I mean, his church, apparently, has now disowned him. But talk about this sexualization of Asian women. Seven of the eight victims were women. Six of them were of Asian descent.
VIET THANH NGUYEN: Well, as so many Asian American women have already spoken about, the question of racism and sexism cannot be separated. So, even if he might have been sexually addicted, etc., whatever his self-proclamations are, the idea that this somehow is removed from any kind of racist preoccupation is absurd. And again, if we look at the way that Asian Americans and Asians have been depicted and exploited in the American imagination, it’s almost always with the intersection of racism, sexism and labor exploitation. And we see that happening exactly in this context, that he deliberately — that is, the shooter — deliberately picked not just any type of place where he might have expected sexual activity, but very specifically Asian massage parlors. And Asian women and Asian American women have always existed as objects of racialized, sexualized, fetishized fantasies for men of many different kinds of backgrounds. There are deep roots of this in American and European culture.
And, as has come to light, many of these women who were working in these massage parlors — we don’t know whether they were sex workers or not; if they were sex workers, that doesn’t invalidate the fact that they were also victims of racist and sexist violence — but many of them appeared to be women of a marginal economic class who were living and working in these massage parlors. In effect, they were exploited laborers. And all these things are happening at the same time. So, it’s enormously frustrating that the police response and the FBI response has been to try to compartmentalize what has taken place under one category only of sexual exploitation, when in fact all these things are happening at once.
AMY GOODMAN: I want to read from a statement by Kimberlé Crenshaw and The African American Policy Forum. Professor Crenshaw writes, quote, “To say the murderer’s actions were about sexual desire, and therefore not about race, is a fundamental intersectional failure: it denies the racial dimensions of the hyper-sexualization of Asian women, and reproduces the environment that makes Asian women particularly vulnerable to harassment, abuse, and murder.” Professor Nguyen?
VIET THANH NGUYEN: No, absolutely, I think Professor Crenshaw is right here. Again, for many Asian American women, they have a long litany of experiences being subjected to harassment, to catcalls, to sexual invitations, and then, of course, also to rape, sexual violence and marginalization, due to their experiences and representations of being Asian American women.
And it’s pervasive in American popular culture, as well. Certainly, the figure of the Asian or Asian American woman as a sexual object or as a prostitute in sort of the American cinematic fantasy has been with us for a very long time. You know, many, many people have talked about this infamous moment in Stanley Kubrick’s Full Metal Jacket where the marines, on first going to Vietnam, encounter a Vietnamese woman prostitute who approaches them and says, “Me so horny.” That became the line for a 2 Live Crew hit that many of us heard in the 1980s and 1990s, and a line that many Asian American women have been subjected to. So, again, in the experiences of Asian American women, racism, sexism and exploitation have been always mutually experienced.
AMY GOODMAN: Viet Thanh Nguyen, if you can talk further about the history targeting Asian Americans and the violence targeting Asian Americans, going back more than a century?
VIET THANH NGUYEN: Well, I’m coming to you from Los Angeles. And one of the worst mass lynchings in American history happened here in downtown Los Angeles in 1871, when a mob of about 500 white men murdered 17 Chinese men and boys. And this was not an isolated incident. This was taking place throughout the western United States. Even I have learned some of these incidents. Most recently, I’ve learned about an incident in Oregon in 1884 where 34 Chinese miners were murdered.
And so, what happened was that Chinese immigrants had come to the United States to work on the transcontinental railroad, and when their usefulness was expired, they were let go and had to make a living for themselves in the American West. And anti-Chinese fervor among the white working class was encouraged by the media and by politicians — again, scapegoating an Asian other in the United States to deal with white working-class economic frustration.
And other Asian populations that came after the Chinese were also subjected to these kinds of feelings. Obviously, there was the Japanese American internment, when 120,000 Japanese American people, many of them citizens, were put into concentration camps, even though people of German and Italian descent were not.
Racist incidents against Asian Americans have proliferated in the last few decades, as well, most notoriously the murder of Vincent Chin in 1982. He was a Chinese American who was mistaken for Japanese by two Detroit auto workers who were frustrated by Japanese economic competition, and they beat him to death with a baseball bat. They did not spend any time in jail. In 1989, five Cambodian and Vietnamese schoolchildren were shot and killed in a Stockton schoolyard massacre by a white gunman, which I feel is a direct outcome of the wars in Cambodia and Vietnam that the United States fought. In 2012 — in 2002, I’m sorry, six Sikh worshipers at a gurdwara in Oak Creek, Wisconsin, were massacred by a white supremacist gunman.
And these are just some of the most notorious incidents. But again, throughout American history, from the 19th through the 20th century up until the 21st century, we’ve seen repeated incidents of both singular and mass anti-Asian violence taking place periodically.
AMY GOODMAN: Do you think what happened in Atlanta has to be immediately labeled as, and the alleged shooter charged with, hate crimes?
VIET THANH NGUYEN: I certainly think so. But again, it was shocking to me to read yesterday in The Guardian that Christopher Wray, the FBI director, has said that it’s not conclusive that this was a racially motivated crime. And the Reverend Raphael Warnock immediately said, “No, it is a hate crime,” when we’re looking at this targeted attack, targeted against Asian massage parlors, in which six of the eight victims were Asian women, who were deliberately tracked down. It looks like a hate crime. It smells like a hate crime. It is a hate crime. And I think, overwhelmingly, the Asian American population of this country believes that.
AMY GOODMAN: Let me go directly to what FBI Director Christopher Wray said on NPR on Thursday about the FBI’s role in the investigation into the mass shooting in Atlanta and his thoughts on the motive.
CHRISTOPHER WRAY: We’re actively involved, but in a support role. And while the motive remains still under investigation at the moment, it does not appear that the motive was racially motivated. But I really would defer to the state and local investigation on that for now.
AMY GOODMAN: That was FBI Director Christopher Wray. And this, as Professor Nguyen talked about, was Georgia Senator Reverend Raphael Warnock’s response.
SEN. RAPHAEL WARNOCK: Law enforcement will go through the work that they need to do, but we all know hate when we see it. And it is tragic that we’ve been visited with this kind of violence yet again. And I’m going to be doing everything in my power as a United States senator to make sure that families don’t have to endure this kind of violence in the first place.
AMY GOODMAN: That’s the new Georgia senator, Reverend Raphael Warnock. We’re going to break and then come back to our discussion with the Pulitzer Prize-winning writer Viet Thanh Nguyen, author of the new book The Committed, sequel to his Pulitzer Prize-winning book, The Sympathizer. We’ll talk to him about his new book and also about his use of the word “refugees” — not “migrants,” but “refugees — whether we’re talking about his family coming to this country from Vietnam or refugees from Honduras or Guatemala or El Salvador. Stay with us.